Reduce Your Company’s Risk
of Costly Accidents & Errors
Due to Fatigue Or Compromised Alertness
Condition Assessment For Your Greatest Asset… Your People!
Reduce Your Company’s Risk of Costly Accidents & Errors Due to Fatigue Or Compromised Alertness
Condition Assessment For Your Greatest Asset… Your People!
Assess
Accurately Assess Worker Fatigue, Alertness, & Readiness-for-Work… in Seconds
Reduce
Reduce Costly Accidents & Errors, Production Downtime, and Worker Compensation Claims
Protect
Protect Your Employees, Company Assets, Reputation & Bottom Line
Worker Wellness/Alertness Is Good For The Bottom Line
With Over 90 Million Worker Hours… The ROI Is Clear!
%
Avg. Worker's Comp Claim Reduction
%
Avg. TRIR Reduction
%
Avg. Reduction Of Cost Of Incidents
Across all types of work environments, if your company has risk due to worker fatigue or compromised alertness, we can help.

Physically Dangerous Environments with a Chronic Risk of Serious Accidents and Catastrophic Losses

Work Environments with a High Risk of Habituation & Complacency Including Work Locations Within the Public Sector
Cognitively Challenging, Fatigue-Inducing, High-Stress, High-Stakes Environments

Accidents & Errors Cost Your Company Money, Time, and Your Reputation
- Annual Cost of Worker Injuries to US Companies: $171 Billion*
- Estimated Annual Cost of Data-Entry Errors: $600 Billion
- Annual Cost of Medical Errors: $20 Billion
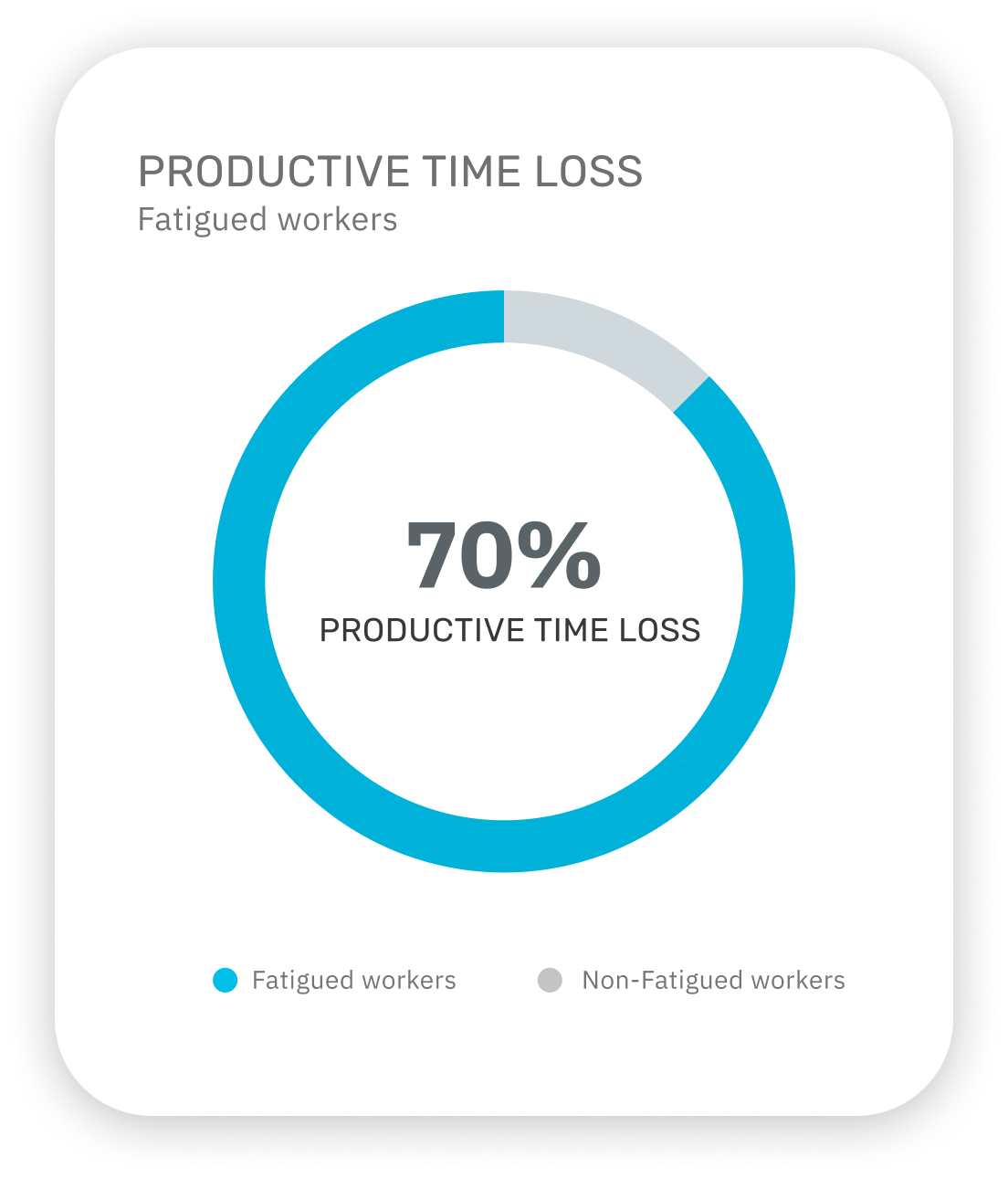
- Productive Time Loss 70% Greater for Fatigued Workers Compared to Non-Fatigued Counterparts
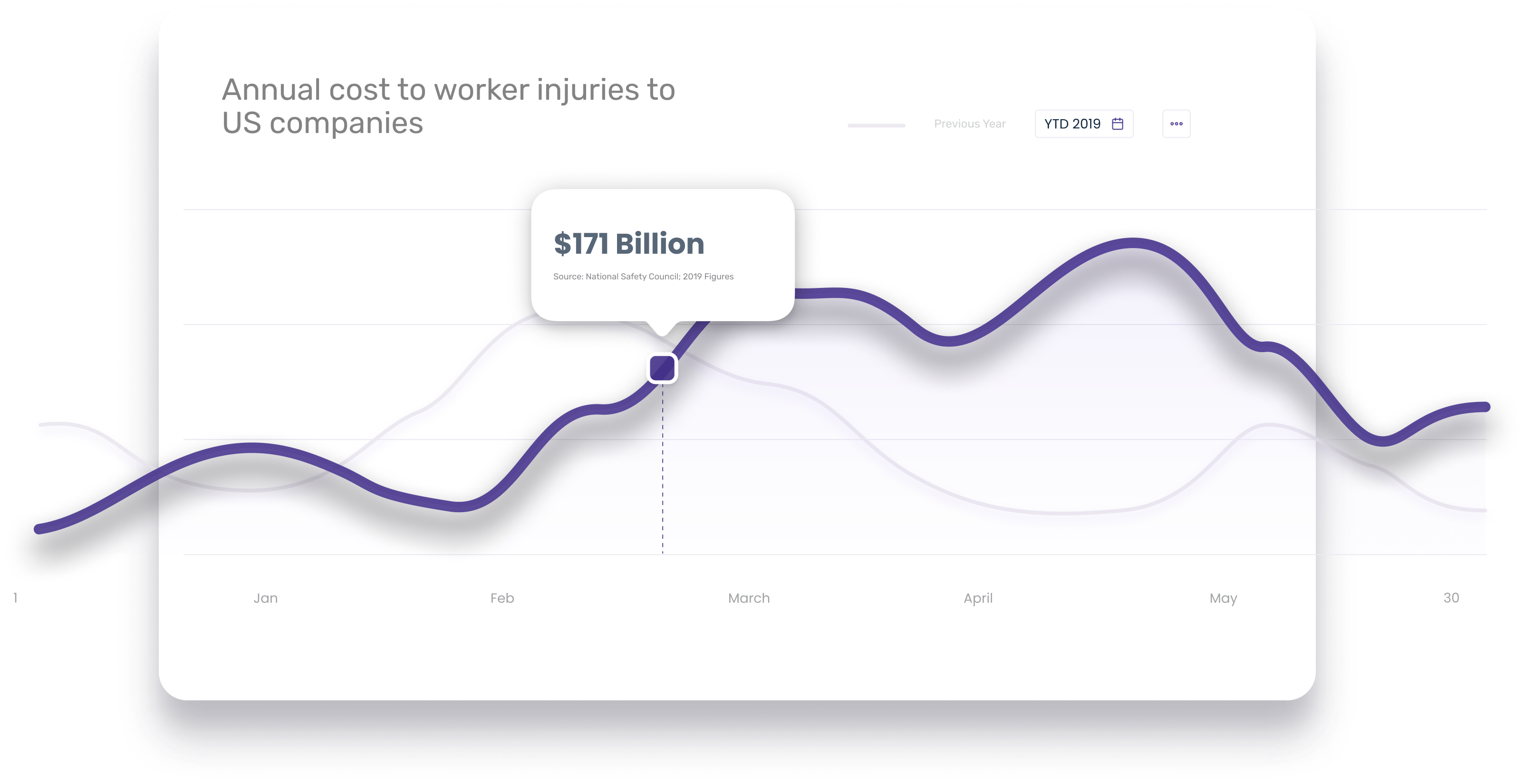



Accidents & Errors Cost Your Company Money, Time, and Your Reputation
- Annual Cost of Worker Injuries to US Companies: $171 Billion*
- Estimated Annual Cost of Data-Entry Errors: $600 Billion
- Annual Cost of Medical Errors: $20 Billion
- Productive Time Loss 70% Greater for Fatigued Workers Compared to Non-Fatigued Counterparts






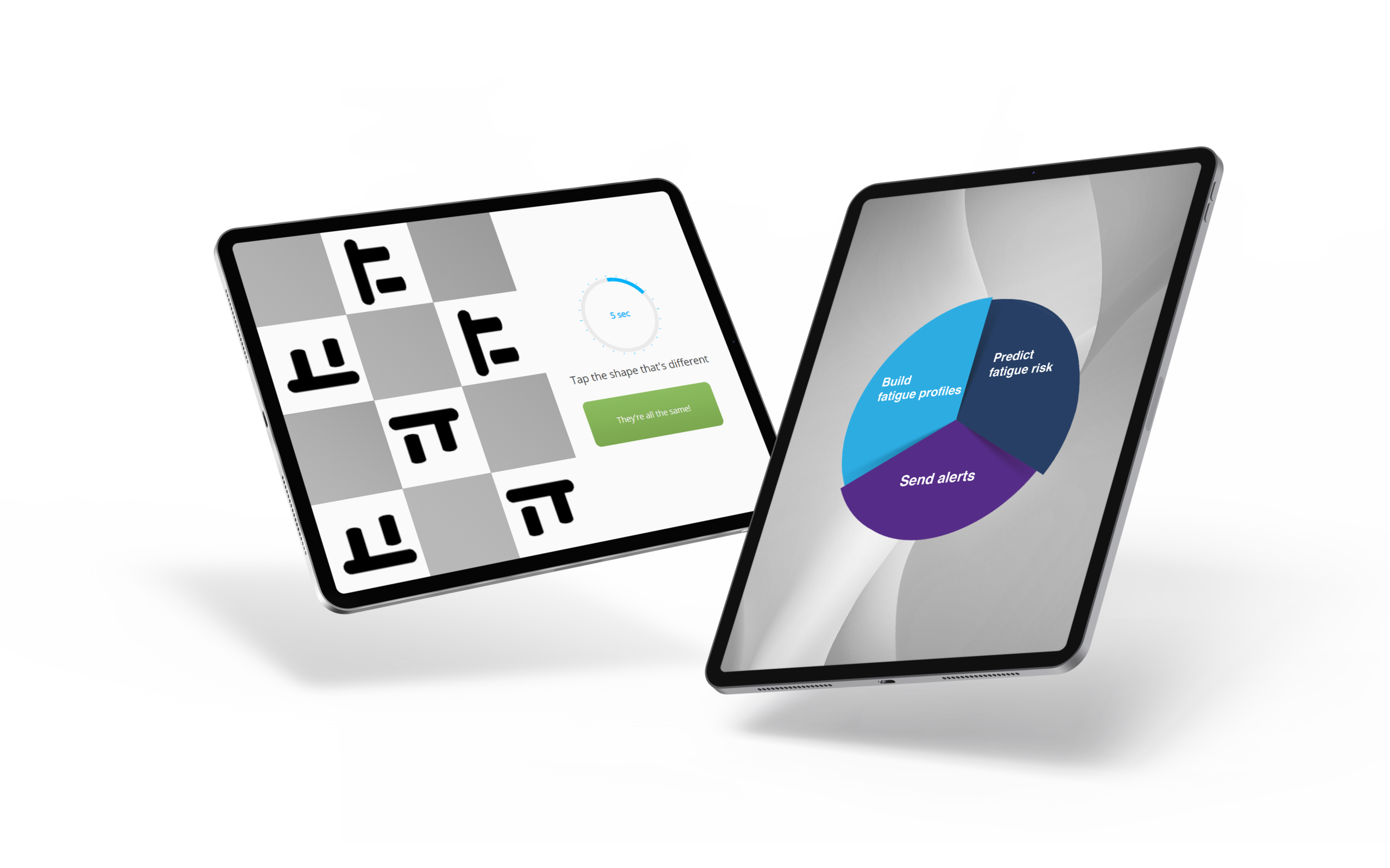



AlertMeter®
- Accurately Track If a Worker is Sufficiently Alert to Perform Their Duties Safely and Efficiently
- Quick, 60-Second Test Can Easily Be Performed Any Time, Any Place
- Game-Like Interface Utilizes Worker-Derived Alghorythm and Can’t Be Cheated
- Objective Results Open Opportunities for Productive Conversations & Create a Collaborative Safety Culture
PRISM™
- See Fatigue Interpreted as Objective Data Giving Supervisors the Ability to Predict, in Real-Time, When Fatigue Progresses to Risk
- Empowers Workers and Supervisors to Engage Time-Efficient and Effective Counter Measures
- Demonstrated to Have a High Level of Worker Confidence and Uptake Helping to Create a Culture of Safety
- May Be Used with AlertMeter® to Provide Individual Fatigue & Alertness Status



Validated in clinical trials
90 million worker-hours tracked
13 patents



Validated in clinical trials
70 million worker-hours tracked
13 patents
Alertmeter’s been a huge asset for us. We have eliminated and reduced the number of injuries we’ve had on-site. We have more confidence that our workforce is ready to work, their minds are in the game, and they don’t have any distractions. I’ve been pleasantly surprised that our employees are also engaged in the process, they have accepted it, and it’s now a culture for us.
General Manager, Triple S
Since getting AlertMeter®, our safety culture has improved. Everyone is looking out for everyone else a little bit more…We’ve really enjoyed it and shown it to some of our friends. Our worker’s comp guys love it.
AlertMeter®’s been great. The platform is really well aligned with our expectations and it allows us to have technology behind what our drivers are doing as well as compliance with DOT requirements.
I am a true believer. The AlertMeter® has been pretty much spot on every time I have been overly fatigued or not feeling well. I honestly found it hard to believe the first few times, but it hasn’t been wrong yet.
Popular &
Current
Explore our wealth of articles and resources that keep you up informed and up-to-date on risk-mitigation, fatigue, impairment and productivity topics that matter to your business.
Service
Innovation
Leadership
Vforge, Inc. management shares how AlertMeter® has reduced incidents and Workers Comp costs and created a Culture of Safety.


Discover How Predictive Safety Can Help You Create a Safer, More Productive Workforce...
Even during a historically tight labor market and high demand.
